I am not a doctor. I did not study neurology past my first-year psychology classes in university, nor do my six years of studying sociology help me to better understand the science behind concussion recovery.
What I do have, is first hand experience of the lack of answers out there for treatment and recovery expectations. Concussion recovery is an ever-evolving mystery that I have been living with since 2012.
If there is someone in your life who has suffered a brain injury, or if you have yourself, I invite you down my rabbit hole.
We’re taking recent research of Traumatic Brain Injuries (TBIs) and Post Concussion Syndrome (PCS) and breaking down the facts, to offer a better understanding of what is going on after a serious blow to the head.
Point of Impact: The Concussion
Concussions are not restricted to athletes, although the sports industry may be the most common place to hear of the injuries. Car accidents, falls, work incidents, and physical violence can all lead to a concussion.
A concussion is the forced impact of your brain against your skull. Considering the plethora of mysteries we have yet to solve surrounding brain function, we sometimes forget how much the brain is affected after a concussion.
All of your senses, thoughts, personality, memories, and basic functioning happen because of your brain. When such a vital organ gets injured and jostled around, there can be devastating effects.
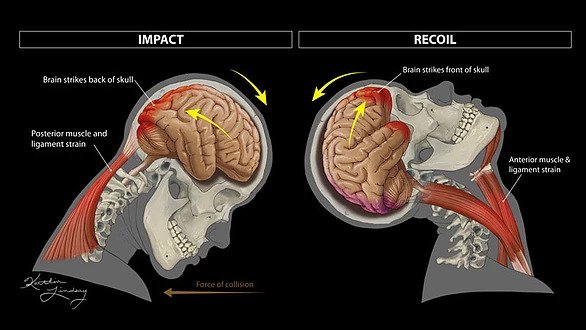
A brain injury can also occur as a result of whiplash. Just because your head did not make direct contact with another object, does not mean you are in the clear.
Whiplash causes hyperextension and hyperflexion in your neck within milliseconds.
This rapid bending to your neck’s extremes not only causes neck injuries, but as the head is thrown backwards, your brain collides with the front of your skull, resulting in injury to the frontal and temporal lobes.
When your head is thrown forwards, the opposite occurs, and your brain collides with the rear of your skull which can injure the occipital lobe and cerebellum.
It is important to note here that every incidence of whiplash does not bring a concussion, and this should in no way be used as a tool for diagnosis.
Now for those of us who no longer remember high school biology, the frontal lobe controls writing, speaking, personality, behaviour, concentration, problem solving, and motor control (so only minor importance, right?).
Your temporal lobe is responsible for comprehension of languages, memory, sequencing, and hearing.
Meanwhile, your occipital lobe interprets your vision for movement, light, and colours, and your cerebellum controls balance and coordination.
When seeking diagnosis of a concussion, not every doctor will have the same protocol, so I will be discussing only what has been most common in my geographical area.
If there has been a loss of consciousness, it is advised to seek immediate medical attention. However, the official ‘concussion’ diagnosis may not be given unless symptoms persist beyond 48 hours.
Again, this is not medical advice nor is it official protocol, so if you experience something different, don’t be alarmed.
The severity of a concussion has changed in name several times over the years, and so you may find two different doctors use different scales.
A scale commonly referred to in the past was mild, moderate, and severe concussions. This was also translated into ‘grades’:
Grade 1: no loss of consciousness, and either no memory loss or memory loss that subsides after 30 minutes
Grade 2: loss of consciousness for under five minutes; memory loss anywhere between 30 minutes and 24 hours
Grade 3: loss of consciousness for more than five minutes and/or memory loss lasting longer than 24 hours
This grading system has changed since its conception in 1998, and some medical professionals choose to disregard the scale entirely, and instead choose to simply diagnose brain injuries as either a concussion or a TBI.
Now, is there a real difference between the two? No. A mild Traumatic Brain Injury (mTBI) is just a fancy way of saying concussion.
Since there is no official grading scale for brain injuries, and what new research determines is in constant flux, there is not going to be a consistent measurement or diagnosis.
Surprising to some, 90% of diagnosed concussions do not involve a loss of consciousness. This means that just because you didn’t pass out doesn’t mean you should not take your hit to the head seriously.
Some TLC: Concussion Recovery
If you thought defining a concussion was difficult, now is a great time to grab a snack and get comfy.
With all the uncertainty that still surrounds the brain and its three-pound grey and white mysteries, it isn’t surprising that treating brain injuries is like playing leapfrog with a unicorn.
There are some myths surrounding the do’s and don’ts of concussion recovery. The key to remember is to treat your brain injury like a really bad muscle injury. If you can’t put weight on your ankle at all, you aren’t going to play in your soccer game tonight. If you do, you’ll find out rather quickly just how bad of a decision that was, and your injury will feel worse.
The same thing happens with your brain; the problem is that we use our brain for e-v-e-r-y-t-h-i-n-g.
Dimming any screens, wearing sunglasses indoors, earplugs, and taking a lot of naps are all common in the days after your concussion.
It used to be taught that sleeping immediately after a concussion was the worst possible course of action, however recent studies have shown that the more you let your brain rest, the better! Yes, that does mean daytime naps – yes, it is glorious.
In the past, it was also thought that exercise was detrimental to concussion recovery.
Recent studies have actually found that exercise does not lengthen recovery time in athletes with concussions, and researchers from Ohio University Heritage College of Osteopathic Medicine found that those who exercised during their recovery had a shorter time span between seeking medical attention and recovery (you can read more about their research here).
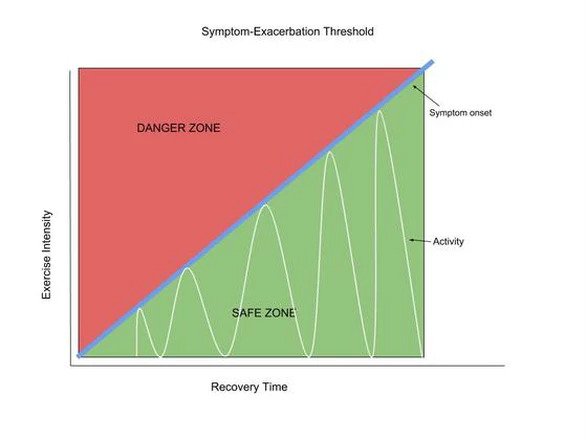
This, and other similar research, was used in the new guidelines from Concussion in Sport Group, saying that “patients can be encouraged to become gradually and progressively more active while staying below their cognitive and physical symptom-exacerbation thresholds.”
Start slow, and don’t continue to exercise once your symptoms begin to increase.
If you are cutting grass or shovelling snow and you have an onset or worsening of symptoms, do not continue to exert yourself. Rest, to allow your symptoms to subside.
Vestibular physiotherapy is a great plan of treatment for post-concussion rehabilitation. It deals with eye movements, eye tracking, balance, and motion sensitivity. Your vestibular system senses linear and angular speed, head movements, as well as sensing your head’s actual position in relation to the space around it.
The most common symptoms for post-concussion clients seeking vestibular physiotherapy include dizziness, nausea, problems with balance, headaches, blurred vision, and sensitivity to visual motion (eg. motion sickness).
Vestibular treatments can include head eye coordination exercises, eye tracking exercises, ocular-motor exercises (which help your ability to look quickly from different targets and your ability to turn your eyes inwards to look at an object), and balance exercises.
Below I have added some pictures of a few of the more common exercises for vestibular physiotherapy.
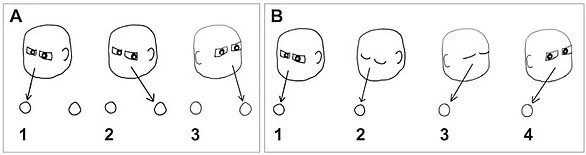
Here we have two objects or targets where you first practice moving your eyes from target to target without moving your head.
The second part of the exercise is to look at the first target, close your eyes and turn your head, then open your eyes to look at the second target.
As is true with all of your concussion rehabilitation exercises, once your symptoms increase, stop.
Time how long it takes your symptoms to return to ‘normal’ or your ‘base’. Ideally, in time, it will take less and less time for your symptoms to go away.
This is the infamous Brock String.
Holding one end of the string against your nose, and the other either tied to a stable object or attached to a wall, the beads are spread along the string at various intervals.
The goal is to be able to shift your focus to each bead without feeling like you are going to vomit or have your head implode.
Feeling like you just stepped off of a roller coaster or wanting to hit your physiotherapist may also be experienced with this exercise.

In this exercise, you hold the paper a fair distance from your face and start looking at the letter A.
You want your eyes to track A,1,B,2,C,3, and so on. I find it helpful to say it out loud as I go, that way I know I am doing it in the right order (we hope).
The Happily Ever After: Maybe
For roughly 80% of people, your concussion will be fine after 7-10 days. The remaining 20% often recover within 3 months or less.
What happens after that three months is often determined by how many concussions you have suffered previously.
In short, if you’re going to hit your head, don’t. If a life-changing experience is what you’re looking for, go do some serious volunteering.
We are talking about leapfrog over a freaking unicorn people.
When you have at least 3 symptoms persisting past the 3 month threshold or your Doctor’s expected time of recovery for you, we welcome you into the PCS family (again, this is more of an observed guideline not a rule, and can change depending on the doctor).
Post Concussion Syndrome (PCS) is like permanently housing the Dursleys. The symptoms go far beyond physical difficulties like vomiting, balance, dizziness, light/noise sensitivity, and headaches.
There are cognitive symptoms such as difficulty concentrating, memory, or feeling slowed down.
My personal favourite cognitive symptom is ‘feeling in a fog’ which is something that makes zero sense until you experience it for yourself.
A friend once shared a video that explained it as ‘staying awake for three straight days then trying to calculate advanced quadratic equations’ – I had always just described it as feeling drunk when you’re completely sober.
Beyond physical and cognitive, there are sleep problems and emotional symptoms. Feeling more emotional or irritable are also symptoms of PCS, as are anxiety and depression.
If you suffered from mental illness prior to your concussion(s), do not be alarmed if your mental health declines.
Speak with your support systems and doctors, and make sure you stay on top of it. Just know that you are absolutely not alone, your PCS family has been (or is still) there, and you WILL be ok.
If you need someone to talk to or having trouble coping with your mental illness call, 1-844-437-3247 (Waterloo-Wellington Region) or visit http://www.yourlifecounts.org/need-help for the list of international support lines.
I was diagnosed with PCS in 2013, and have used way more sticky notes since then than I had ever thought possible.
However, just because I have been dealing with this for the past five (+) years does not mean I have not shown significant progress.
Below I have added a snapshot of where I was at in 2015 after I was hit in the head again, versus where I am today.
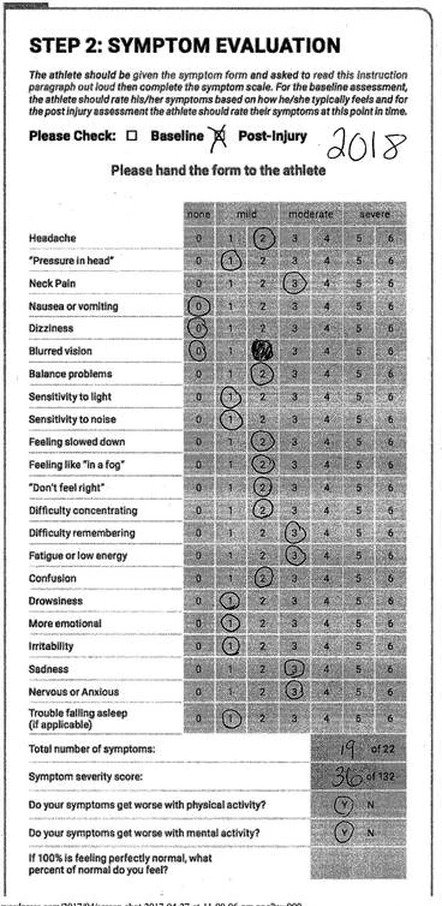
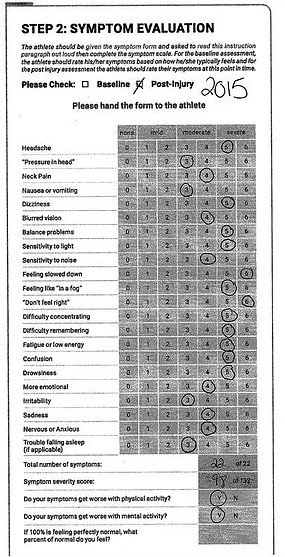

This progress was not miraculous, nor did it come easy.
Physiotherapy takes a lot of hard work, and you have to commit to your exercises.
Since 2013, here are the tricks and treatments I found worked best for me (again, not a doctor, this is not medical advice):
- Vestibular physiotherapy
- Acupuncture (points used were LI4, GV24.5, GV26, EX-HN5, ST44)
- Massage therapy (neck and shoulders)
- Chiropractor
- Peppermint essential oil (on each temple and along your hairline on the back of the neck to relieve headaches)
- Omega-3 Fish Oil
- Melatonin (to aid in regulating sleep, not taken long term)
- Naproxen (for stronger headaches and migraines)
The emotional side effects of PCS are by far the most difficult to deal with.
Accepting that the person you used to be is no longer the person you are, is incredibly difficult. (You can read more on that here).
Once you have overcome this incredibly difficult challenge, you then have to re-introduce yourself to your friends and family.
No part of PCS is easy or simple, nor should we expect it to be. Our brains are still an area where we have only scratched the surface of understanding.
Recovery from a head injury is complex, and no singular solution is going to work the same for each person.
It is incredibly frustrating to not have a solution to a problem, especially when it concerns your health.
Unfortunately, this is a reality we face with PCS. The best thing you can do is be aware of your limitations, track how your symptoms are doing day-to-day, and work with your trusted health professionals.
If you plateau, or stop showing signs of improvement, don’t give up! The brain can do a lot of incredible things, and it may take its sweet time to recover.
[Update:] Even after 5 years since my last major injury, I am still working towards improvement. I’ve been reintroduced to physical activity! A huge deal for me. You can even follow along with me as we try to work me up to running again!
My main advice: take preventative measures, be cautious. Do not hit your head again. (Coming from the girl with double digit concussions…)
Still not sure what your findings mean, or what to expect with your injury? Call us at 519-895-2020, or use our online booking tool on www.strivept.ca to book an appointment with one of our knowledgeable physiotherapists, and they will be sure to help you understand your injury.

Best of luck on your road to recovery,
Chelsea Simo
Strive Physiotherapy & Performance