If 16 years of dance taught me anything, it was to suck it up and dance through the pain. Smile and show no weakness, and worry about it when the performance is over and you are off stage.

Just don’t think about it until the curtains close, right?
But look at me now! A retired dancer whose body feels twice as old as she is.
Now that my ‘young and naive’ years are behind me (or at least the naive part, we hope), let me share some of my infinite wisdom with you: how we tend to treat our bodies, especially in the higher levels of dance and gymnastics, is. not. healthy.
It may seem like the industry standard to keep training after an injury, but not giving your body the proper time to recover will only increase your chance of reinjury, and ultimately take longer to heal in the first place. No matter how dedicated and determined we are to keep pushing through, we need to stop and put our bodies first.
Fear not! I’m not writing this post to scold you on how you treat your body. I completely understand the risk vs. reward of high level competitions.
Instead, I have compiled a list of the 10 most common injuries we face as competitive athletes in our sport. As gymnasts also have a lengthy list of wrist and shoulder risks, I have limited this list to just lower-limb injuries that are common across the board.
These are the injuries that physiotherapists see alarmingly frequently, as well as what I have seen (and experienced) the most as both an athlete and a coach. With the help of the physiotherapists from Strive Physiotherapy & Performance, I’ve also included not just treatment, but also prevention techniques so you can help prevent these injuries in the first place.
So without further ado, let’s jump in!
1. Anterior Cruciate Ligament (ACL) Tears
- What it is: Your ACL is what runs through your knee to connect your thigh to your shin (connecting your femur and tibia). It plays a key role in the stabilization of your knee. The full name is your Anterior Cruciate Ligament. When this tears, the ligament quite literally rips in half.
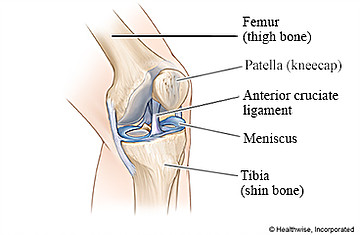
- Common Symptoms: When a ligament tears, especially one of this size, you will hear a ‘pop’ at the time of the injury. This will come with severe pain, swelling, inability to put weight on that leg, and a significant change in your range of motion.
- Treatment: It depends on the significance of the tear. With grades I and II tears, the treatment usually focuses on progressive range of motion, strengthening, and motor control exercises. Treatment will also aim to address the possible causes of your injury (see Prevention Tips). With grade III tears (ACL ruptures), a surgical consult is often recommended, and 9-15 months of progressive rehab will take place after surgery.
- Prevention Tips: Address the modifiable risk factors, which may include: body-mass index (higher BMI = higher risk), jump landing mechanics, muscle imbalances (quadriceps to hamstring ratio often imbalanced), hormonal imbalances, or overtraining.
- Key muscles to target: hamstrings and gluteals (especially lateral gluteals)
2. Achilles Tendon Strains, Tears, and Tendonitis
- What it is: Your achilles is the longest tendon in your body. It is what lets you point your toes and raise up to the balls of your feet. While quick stops and starts can cause an achilles injury, pivoting is also a common cause.
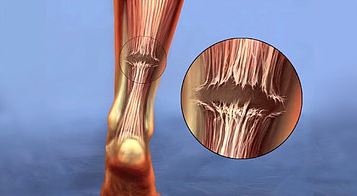
- Common Symptoms: Pain above your heel, particularly when pointing your toes can be a sign of an achilles injury. For more severe injuries such as a rupture or a tear, you may feel immediate and sudden pain, along with a popping noise, bruising or swelling. Tendonitis of your achilles refers to an overuse of the tendon, rather than a strain or tear.
- Treatment: Rest is usually a good starting point, and the Achilles is often offloaded initially (i.e. with a heel lift). Rehab will focus on calming down the pain, then building the tendon strength back up. You will learn how to make your Achilles’ tendon very strong and capable of all types of load (like jumping or running loads). Heel raises will become your new best friend.
- Prevention Tips: Rest when you feel any pain starting in your achilles or heel, and see a physiotherapist for a proper assessment. Ensure you have excellent calf strength (heel raises are helpful!), and make sure your calf is loose (massage, foam roll, and stretch!). When sitting or not at dance, don’t point your toes all the time.
3. Ankle Sprains
- What it is: There are three ‘grades’ of ankle sprains: grade 1 involves mild pain and swelling with minimal to no loss of function, grade 2 involves moderate pain and swelling with some bruising and instability, grade 3 involves lots of swelling and bruising, complete loss of function, and often a complete tear. After your first sprain, you are twice as likely to sprain that ankle again in the future.
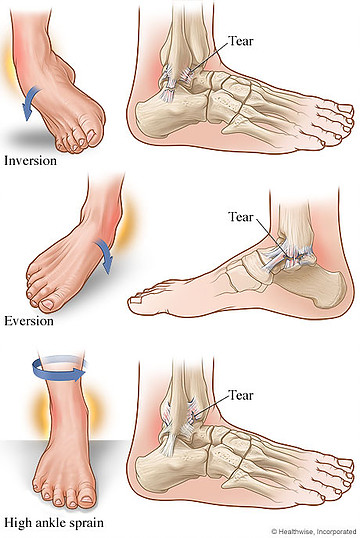
- Common Symptoms: pain over top of your ankle ligaments (most commonly, the outside of the ankle), which is increased if you stretch the ligament. It often hurts to walk (but you should still be able to), and it’s usually painful to move your ankle around, or climb stairs.
- Treatment: Dependent on the severity of the sprain… but usually, a day or two of rest, but then get straight back to using your ankle slowly and safely. You can ice for the first day or two to help with pain, but in the majority of cases, gentle movement, heat, and compression and/or bracing works best.
- Prevention Tips: There’s evidence to support the use of bracing and taping to prevent ankle sprains. Otherwise, you want to ensure you get proper rest, sleep, and nutrition, while ensuring you have great single leg balance/control and good lower extremity (hip, knee, ankle, and foot) strength!
4. Ankle Impingement
- What it is: ankle impingement can happen anteriorly (on the front) or posteriorly (on the back) of your ankle. It occurs when soft or bony tissues get compressed within the ankle joint, usually at the extremes of range of motion (like pointing your toes really far). It is often a repetitive stress injury.
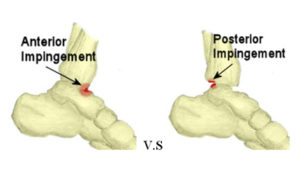
- Common Symptoms: the location of the pain can help determine the type of impingement. Anterior ankle impingement hurts on the front of your ankle, usually with activities that cause deep dorsiflexion (bending the foot up). Activities include jumps, squats, or going down stairs. Posterior ankle impingement hurts on the back of your ankle, usually with activities that involve pointing your toes. Some people even have an extra little bone on the back of their ankle (called an ‘os trigonum’, which can lead to these posterior impingement symptoms.
- Treatment: decreasing the activities that aggravate your symptoms will help in the early stages of rehabilitation, as there’s often an inflammatory process that needs to calm down. After that, a slow, progressive strength and balance program will begin, which is geared at getting you back to doing the previously-irritating activities. In some cases, ankle bracing can be helpful while you learn to improve your ankle control.
- Prevention Tips: deal with any previous ankle injuries as soon as possible. It is believed that repetitive ankle injuries (like sprains) can lead to an ankle instability that plays a role in ankle impingement. Poorly healing sprains can also lead to hypertrophic (bigger) scar tissue formation which takes up more space in your ankle joint. Otherwise, prevention is much the same as the other ankle injuries – get proper rest (especially if you feel pain starting), sleep, and nutrition, while ensuring you have great single leg balance/control and good lower extremity (hip, knee, ankle, and foot) strength!
5. General Knee Pain and Patellofemoral Pain Syndrome
- What it is: pain in the knee that is usually described as “all over”/”general”, or “behind the kneecap”. We used to think that patellofemoral pain syndrome was when your patella (knee cap) rubbed on your femur (upper leg bone), but that doesn’t necessarily have to happen to experience pain, nor is it overly dangerous if it does happen.
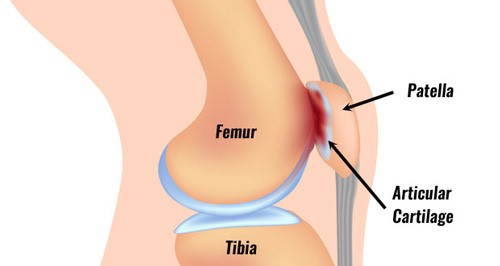
- Common Symptoms: pain that feels general to your knee (notpoint-specific), or behind your knee cap. An ache that usually intensifies during or after activities like squatting, running, or jumping.
- Treatment: Decreasing your activity level can be helpful to calm down the symptoms. Then work on strengthening the muscles around your knee. The hip muscles often also need to be strengthened, because the hip muscles help to control your knee. Foam rolling your quadricep muscle and using heat can be helpful to manage your pain. Using a compression sleeve or brace may also provide you some relief during your practices.
- Prevention Tips: Cross training (participating in more than one sport in a given year) can be helpful to provide a variety of load on your body to keep you strong. However, keep in mind the amount of training that you’re doing – if you’re doing 12 different sports/activities at the same time, your muscles and joints might have a hard time keeping up!
6. “Jumper’s Knee”
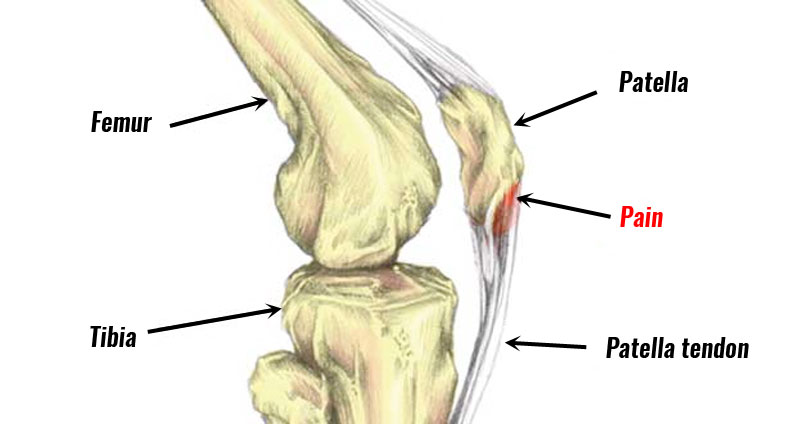
- What it is: Also known as patellar tendinopathy, this is an irritation of the tendon that connects the quadriceps muscle to the lower leg.
- Common Symptoms: Pain inferior to your knee cap, especially with jumping (as the name suggests!) but also with other squatting movements (ie. a plié!)
- Treatment: Relative rest (modifying your practices) is required including limiting jumping and explosive movements. Then you can start strengthening your quadricep muscle which helps to strengthen your patellar tendon. You can also get a Jumper’s Knee brace that can help decrease your symptoms during your practices.
- Prevention Tips: Keep your hip and knee muscles strong and flexible. Take special care during growth spurts when you’re young – these are the times where activity that has previously been fine can be become problematic.
7. Snapping Hip Syndrome (“Dancer’s Hip)
- What it is: Your tendons and muscles moving over the bony areas in your hip. Normally you can’t feel this happening, but it can progress to an uncomfortable sensation or even a painful one. This may happen more during growth spurts, or with an increase in your activity level, especially if it includes lots of hip movements!
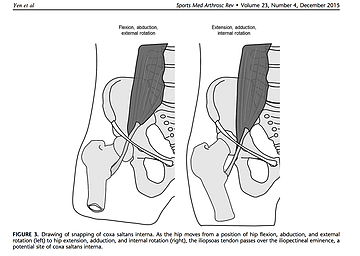
- Common Symptoms: a snapping sensation when moving your leg back and forth, or with circular patterns, that may or may not be painful. If left untreated, the pain may spread to the surrounding muscles.
- Treatment: Decrease your activity level to better manage any painful symptoms. Once the pain is better managed, slowly return back to your usual activities. Meanwhile, work on stretching out your muscles in your legs and your hips and also work on strengthening these same muscles to increase their tolerance for your activity. You may find heat to be relieving.
- Prevention Tips: Foam roll your muscles, especially in times of growth spurts or high activity level. You can also ensure to manage your duration, frequency and intensity of your practices – sudden increases in activity may turn a slight discomfort into pain.
8. Hip Joint Irritation
This can be caused by a number of conditions, including arthritis, labral tears, or cam/pincer impingements
- What it is: exactly what “it” is would depend on which exact condition you have, but in general, the surface of your hip joint is irritated by bony abnormality (cam/pincer morphologies), soft tissue injury (labral tear), or arthritic change. This can cause inflammation and pain.
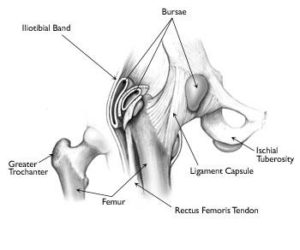
- Common Symptoms: front of your hip pain that feels “deep”. Some describe pain in the groin, or pain that wraps from the front around to the back of your hip. If significant, you will limp, and you will likely have trouble with running, jumping, deep squats, and crossing your legs.
- Treatment: Treatment will require rest to calm the inflammation process, with a slow, progressive build back to aggravating activities. Rehab will focus on building strength and control around your hip and gluteal? musculature, while ensuring as much comfortable range of motion as possible.
- Prevention Tips: ensure you have excellent leg (hip, knee, ankle) mobility and strength. Get plenty of rest and sleep, while identifying aggravating factors early.
9. Stress Fractures
Metatarsals, tibia, sesamoids, and lumbar spine
- What it is: Stress fractures are small fractures that happen in your bones in response to TOO MUCH load. The bones are unable to keep up with the recovery process between sessions and can start to have micro-breaks in the bone.
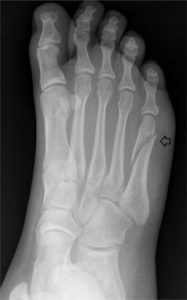
- Common Symptoms: Pain in the area of the stress fractures which feels worse with loading, and feels better if rested.
- Treatment: Rest the area to allow the bone to heal (avoid high impact movements), and then initiate progressive loading to get the area to tolerate your practices again. This may take 1-2 months to get better.
- Prevention Tips: Load appropriately – beware of sudden changes of your activity level in terms of frequency, duration, or intensity of your routines. Ensure you are eating well – proper nutrition is important in your body’s recovery process.
10. Flexor Hallucis Longus Tenosynovitis (“Trigger Toe”)
- What it is: Our tendons have a sheath that they glide through in order to move our bones. If these tendons are overused, this can cause irritation and make the glide through the sheath a little more… stuck.

- Common Symptoms: Your big toe can get stuck in a bent position, and it can be difficult to make it straight again. It can be painful to click back to the normal position. In the early stages you will experience mild pain in the big toe, with brief locking that is easy to unlock. If the condition worsens, the ‘en pointe’ position will be quite painful, and locking will intensify. Often, there is morning stiffness and tenderness, or a ‘clicking’ sound when the toe locks in and out.
- Treatment: Severe cases often require surgery. In order to avoid that, it is important to rest well between sessions, and limit the ‘en pointe’ position when able. Treatment will otherwise focus on reducing inflammation and ensuring full, comfortable toe, foot, ankle, and calf mobility/strength.
- Prevention Tips: Ensure you warm up your toes, feet, ankles, and calves before each session, and stretch gently after sessions. Ensure you have good big toe mobility, and address concerns as soon as you feel pain.
BONUS:
Bunions
- What it is: Also called “hallux valgus”, bunions occur when the joint at the base of the big toe becomes stretched out and possibly subluxed, resulting in your big toe pointing in towards your other toes.
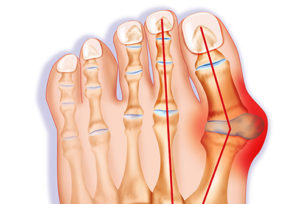
- Common Symptoms: The joint of your big toe may be swollen, painful, and the muscles of the big toe may be weak.
- Treatment: Rest the big toe from aggravating activities like heel raises and doing activities on your toes (yes, that means taking a break from pointe shoes). Then work on mobilizing the joint (restoring the range of motion) and strengthening the big toe muscles.
- Prevention Tips: Avoid wearing narrow toed shoes or excessively tight footwear for prolonged periods of time.
There you have it, common lower limb injuries and tips on preventing them. Best of luck on your upcoming competitions – knock ’em dead!

At Strive Physiotherapy and Performance, we are committed to providing an in-depth assessment to ensure we can work together to find the best plan of action for each individual client. Call us at 519-895-2020, or use our online booking tool on www.strivept.ca to book an appointment with one of our knowledgeable physiotherapists.
Cheers,
Chelsea Simo
Strive Physiotherapy & Performance