Low back pain is one of the more common complaints we deal with at Strive Physiotherapy & Performance.
Often times, our clients will express concern about having sciatica, as they may have had it, thought they had it, or knew someone who had it in the past.
Sciatica is sort of a complicated topic and often times, any back pain, or any leg pain is confused with sciatica.
This blog post aims to clear up a few things about sciatica. We will discuss:
- What sciatica is
- Some anatomy (kind of a theme with my blog posts, isn’t it?)
- Common symptoms and what else it could be
- A few tips on how to manage sciatica, should you unfortunately experience it
What is Sciatica?
Sciatica is a neurological (nerve) problem that occurs when the sciatic nerve is entrapped or irritated.
What exactly does a nerve do? In short, nerves send the signals that are responsible for telling our muscles to move, and for telling our brain how/what we feel.
Having sciatic nerve (“neurological”) symptoms means that you will be experiencing fairly intense pain in the buttock area, and down your leg.
You may also experience 1 or more of the following:
- Numbness and tingling feeling down your leg
- Decreased reflex response
- Muscle weakness (along a myotome)
- Decrease or change in sensation (along a dermatome) (we will discuss ‘myotomes’ and ‘dermatomes’ later)
We will re-introduce these thoughts later on, but first we must set up a baseline understanding.
Anatomy
The sciatic nerve is big, and it covers a lot of ground within our bodies. In fact, we have 2 sciatic nerves, one for the left low back and leg, one for the right low back and leg.
Our lumbar and sacral spines have 5 nerve roots each (labeled L1, L2, L3, L4, and L5; S1, S2, S3, S4, and S5).
Each sciatic nerve comes from 5 different nerve roots within the lumbar and sacral spines. Our sciatic nerves branch from L4, L5, S1, S2, and S3 on each side.
Like this:
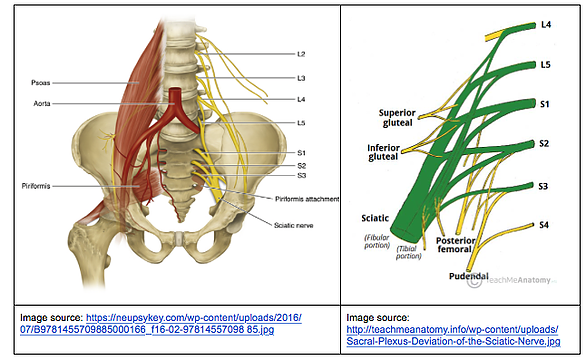

The picture on the left is a front view and shows the left sciatic nerve coming off of the lower 5 nerve roots (L4-S3).
It also shows a ‘piriformis’ muscle (remember that for later!). The picture on the right shows how the 5 nerve roots (L4-S3) come together to make the sciatic nerve (big green one!)
Although those 5 nerve roots come together to make 1 sciatic nerve, our bodies tend to keep track of each nerve root. We know that because we have ‘myotomes’ and ‘dermatomes’. A group of muscles that are supplied by a single nerve root is deemed a myotome.
A dermatome is an area of skin that is mainly supplied by a single nerve root. Here are some examples:
- Your L5 myotome is lifting your big toe up
- The sensation on the skin down the side of your leg and wraps onto the top of your foot to your big toe is your L5 dermatome (you’ll see a picture later in this post)
This is important because sciatica pain typically follows a dermatomal pattern, and you can also have weakness in 1 or more of your myotomes (aside: you might also have decreased reflexes along a nerve root pattern!).
Most common sciatica symptoms:
Much like almost every injury, each sciatica case can present somewhat differently. That being said, the most common symptoms include:
- Pain (the hallmark symptom)
- Can be sharp, electric shock-like, numb, or achy
- Constant or comes and goes
- Is along the distribution of the nerve (in the back, buttock, and leg) (remember the dermatomes!)
- Is almost always only down 1 leg, not both
- Usually, the pain goes past the knee
- Walking difficulties
- Decreased or different sensation along the dermatome
- Decreased power in the leg
- Decreased reflexes
What can cause sciatica?
Many different things can cause sciatica. Some of the more common causes include:
- A disc herniation or protrusion that can press on the nerve (most common) (and don’t worry, a disc herniation is often less scary than it sounds!)
- Spinal stenosis (narrowing of the gaps in your bones where the nerve passes through)
- Swelling in the area of the nerve from a fall or contusion
- Pressure on the nerve from a variety of sources – for example, by growing a baby (pressure from the inside)
What else could it be?
Sciatica can sometimes be misdiagnosed, which is why it’s important to get a proper assessment. Other possibilities include:
- Mechanical low back pain
- Muscle strain – in the leg or back
- Vascular problem – such as claudication (blocking of a blood vessel)
- Piriformis Syndrome
The last one, piriformis syndrome, has many of the same symptoms as sciatica, so I’ll try to differentiate things a little bit.
Both sciatica and piriformis syndrome will present with a variety of symptoms including back/buttock/leg pain, numbness/tingling, and/or walking difficulties.
Here are some differentiating features:
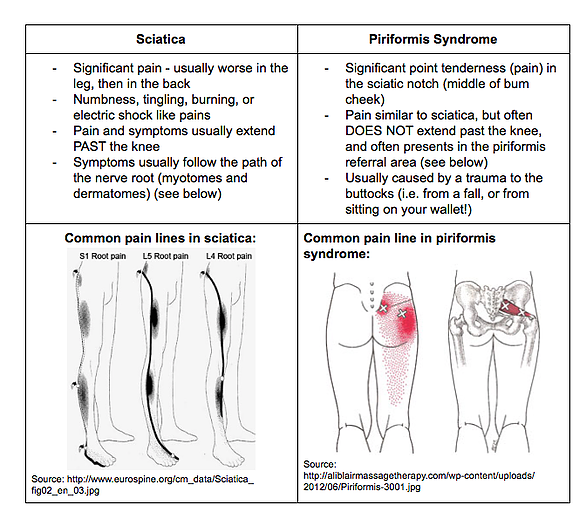
What can I do about it?
First and foremost, it is important to have your pain and injury assessed by a healthcare provider you trust.
Sciatica can come from a variety of sources, and it is important to try and determine the most likely source.
This is because, depending on the source, the management can be completely opposite. For example, if you have sciatica due to a disc herniation pressing on the L5 nerve root, then you will likely prefer extension-type exercises.
However, if you have sciatica from spinal stenosis, then you will likely prefer flexion-type exercises. Additionally, if you do the opposite exercises than what would be most preferable, you may actually make yourself worse!
If you think you may have sciatica, one exercise you can do to try and improve how well your nerve is moving is called a sciatic nerve floss.
Here’s a good video of a sciatic nerve floss:
Remember to look up as you bend your foot, and look down as you straighten your foot.
Timing is important, and doing it opposite (i.e. bending foot up while looking down), can make you more irritable.
You should only complete this exercise if it feels relieving or if it feels like a “nothing” feeling. If it hurts, stop, and consult your physiotherapist.
How do I know if I’m getting better?
I will try to keep this section short and sweet. If you’re getting better, your pain will be lessening in intensity and frequency, and you should be finding it easier to move around (walk, get out of bed, etc).
One important thing to note is that as you heal, your pain will likely centralize towards your back (i.e. move UP your leg).
This is a good thing. The downside, however, is that it might make you feel more intense pain in your bum or back.
That being said, as long as you have less (or no) pain further down your leg, that’s actually ok!
Conclusion
Sciatica is a painful neurological (nerve) injury that usually affects only one side of your back and leg.
There are many potential causes of sciatica, and many other things it could actually be, meaning it’s important to get a detailed assessment.
Do you think you have sciatica?
Are you interested in decreasing your pain?
At Strive Physiotherapy & Performance, we are committed to providing an in-depth, one-on-one assessment to ensure we can work together to find the best plan of action for each individual client.
Call us at 519-895-2020, or use our online booking tool on www.strivept.ca to book an appointment with one of our knowledgeable physiotherapists, and they will be sure to help you understand your injury.
Take care,
Tyler Allen
Physiotherapist at Strive Physiotherapy & Performance