Pain is the most common reason someone sees a physiotherapist.
How pain impacts a person’s identity, their relationships and their outlook on life, are typical factors for an individual to seek counselling support.
Consequently, pain is one of healthcare’s greatest challenges. We’re literally spending billions of healthcare dollars on pain management without a true solution to the problem.
Why isn’t there a solution?
This is because pain is individualized. You could have 5 people with the same injury and they will all present differently, with different amounts of pain.
Their bodies will all react differently to the same approach. Conversely, their brains will react differently too.
For some, pain may be seen as a challenge that needs to be tackled and overcome, for others it may be perceived as a threat that is robbing them of their person-hood; both mindsets can be detrimental to recovery.
Whether it be stress and frustration adhering to the slower pace an injury demands or overcoming anxiety and fear as the result of an injury,
These are just two examples in a multitude of ways people comprehend pain. Interestingly, most people believe pain is experienced the same way by everyone, like we’re cars made on the same factory line.
There is a belief that we all heal the same way and that the same therapeutic approach works for everyone; a one size fits all. If this were the case,
North Americans wouldn’t be spending approximately $600 billion dollars per year toward the care and management of chronic pain.
For practitioners and the healthcare system as a whole, this is where the challenge lies.
New research over the past 5 to 10 years has shown that pain depends on many factors.
One small factor is your actual injury.
Your actual injury may cause pain, but did you know that within 15 seconds of experiencing pain your brain changes the way it thinks about an injured area?
So, if you hurt yourself reaching for a cup of coffee, your brain will think differently about how to reach for a cup of coffee while you’re experiencing pain.
If you don’t recover from your injury, this new pathway can create adaptations in your brain that modifies your body and movement compared to how you moved before you experienced your pain. Check out this amazing video from one of the world’s leading pain researchers.
Now, let’s take it a step further. Research also indicates that your experience of pain is greatly influenced by your current and past experiences with pain,
Your ability to cope and manage with emotional responses to stress, your work-life balance, your support system and much more.
This is called the biopsychosocial model of pain. Considering all these factors, can we really attach all of our focus on our tissues as the main or only source of our pain?
The more we learn the more we can confidently say
“No”
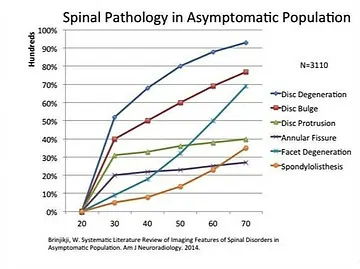
In fact, through medical imaging, researchers have found that people can have disc bulges, meniscal tears, osteoarthritis, and many other diagnostic findings without the experience of pain.
There have been multiple reports that show people without pain having the exact same MRI findings as someone with pain.
Check out the findings comparing MRIs for people with and without low back pain.
Can this go both ways?
If we can be pain-free regardless of a muscular, tissue or skeletal change in our body, can we experience pain when there is no longer a tangible change in our physical structure?
Totally!
There are many people that experience pain for years following an injury, but their injury has been fully healed. So how do they still experience pain?
Current science indicates that all the other factors discussed above may continue to influence pain for years following an injury and lead to a life with chronic pain.
You may want to ask yourself the following: Have I returned to sleeping well following my injury?
Am I avoiding certain movements? Is the pain I’m experiencing hurting a relationship at work or at home? Does my pain lead to feelings of fear or anxiety in certain situations?
Check out this video about how pain can be impacted by our daily lives.
What does that mean?
It means we believe you can get better. It means that we don’t take a “one size fits all” approach to your pain but rather an integrated look at what could benefit you.
It means with the right approach we can calm things down and build them back up. It means we can retrain your brain to overcome pain and return to previous levels.
Are you looking to find out more?
At Calming Tree Counselling and Strive Physiotherapy & Performance, we’re committed to providing a multi-disciplinary and in-depth assessment to ensure we can work together to find the best plan of action for each individual client.
Have a great day,
Mike Major, Physiotherapist at Strive Physiotherapy & Performance,
and Melissa Reid MSW, RSW at Calming Tree Counselling
About the Authors:
Melissa Reid is a Registered Social Worker with a Master’s degree in Social Work. Ms. Reid received her undergraduate degree from the University of Waterloo after which she pursued a certificate in child abuse studies, and finally a Master’s in Social Work from Wilfrid Laurier University, Waterloo, Ontario. Ms. Reid has also participated in numerous educational conferences on trauma, grief and bereavement.
Mike graduated from the University of Waterloo in 2006 with an Honours Bachelor of Science in Kinesiology. Immediately upon graduation, he was accepted into McMaster University’s Physiotherapy program where he graduated with a Masters of Science in Physiotherapy in 2008. Prior to becoming a physiotherapist, Mike served in the reserves for 9 years as a member of the Artillery in the Canadian Armed Forces.