When you injure your knee, you can be suddenly bombarded with foreign words and acronyms that don’t mean a whole lot to you. ACL, MCL, PCL, LCL, meniscus, patella…
Now despite the knee joint being fairly simple in how it moves (bends and straightens) – a lot of structures make up a healthy knee joint.
As knee injuries are fairly common, I wanted to write a quick post explaining what structures are part of your knee joint, and what these structures do.
I’ll even include information about common injury mechanisms and rehabilitation.
The Bones:
The bones of the knee joint are fairly straightforward.
You have a femur (upper leg) bone that meets with your tibia (shin) bone, and a patella (knee cap) over top of where the femur and tibia meet.
Finally, there is a second lower leg bone on the outside of your leg, called your fibula. See the picture below (right knee):
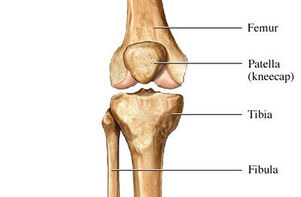
The Ligaments:
We’ve learned in previous blog posts that ligaments connect bones to bones.
They are passive structures (we can’t control them with our minds) that hold bones together.
This is where those acronyms come in – ACL, PCL, MCL, LCL – so let’s clarify. The ACL and PCL connect the femur and tibia on the INSIDE of the knee joint.
The MCL and LCL connect the femur and the tibia/fibula on the OUTSIDE of the knee joint.
- ACL stands for Anterior Cruciate Ligament
- The ACL connects from the posterior (back) part of femur, to the anterior (front) part of the tibia – on the inside surfaces.
- The ACL stops the lower leg bone (tibia) from translating forward too far on the upper leg bone (femur).
- This ligament is commonly injured when the foot is planted on the ground and a direct (i.e. someone tackles you), or indirect (i.e. fast twist/landing from a jump) force is applied to the knee while the leg is straight or slightly bent.
- When this ligament ruptures completely, you usually hear/feel a “pop”, and swelling starts almost immediately.
- PCL stands for Posterior Cruciate Ligament
- This is the opposite of the ACL, and it connects from the anterior (front) part of the femur, to the posterior (back) part of the tibia – on the inside surfaces.
- The PCL stops the upper leg bone (femur) from translating forward too far on the lower leg bone (tibia).
- This ligament is rarely injured, and most commonly happens when the tibia is forced backwards on the femur when the knee is bent (i.e. the front of your bent knee hits the dashboard during a car accident).
- MCL stands for Medial Collateral Ligament
- The MCL connects on the inside (medial side) of your knee. It connects the femur and tibia together. Some fibres connect to your meniscus (more on meniscus later).
- The MCL stops your tibia from bending outwards on your femur (resists ‘valgus’ forces)
- This ligament is commonly injured in similar ways to the ACL, or when the leg is forced into ‘valgus’.
- LCL stands for Lateral Collateral Ligament
- The LCL connects on the outside (lateral side) of your knee. It connects the femur and fibula together.
- The LCL stops your tibia/fibula from bending inwards on your femur (resists ‘varus’ forces)
- This ligament is not commonly injured, but happens when the leg is forced into ‘varus’.
Here’s a good picture of the ligaments (right knee, with the knee cap removed):
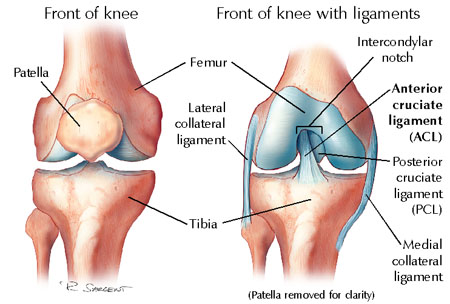
The Menisci:
The menisci (plural of meniscus), can be visualized as little cushions between the tibia and femur bones.
They are shaped like C’s, and help to disperse the forces in our knees. See the photo:
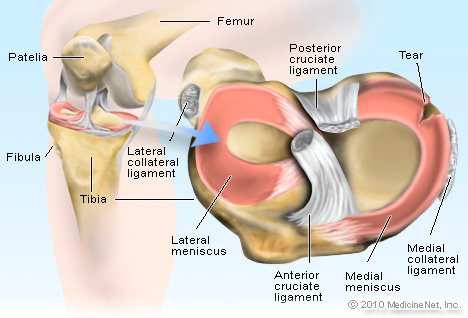
As you can see in the photo, the menisci sit on the tibia bone. As mentioned, their function is to help cushion the knee, and disperse the forces applied through the knee.
They also provide stability to the knee joint and reduce friction. With a meniscus injury, swelling typically starts hours after the injury, not immediately, like with an ACL injury.
Meniscal injuries often happen when twisting a bent knee (especially if fully bent), or with foot-planted knee twisting.
Some happen from direct trauma to the knee. If you have damaged your meniscus, you may feel like your knee catches or locks when you bend and straighten it.
It may also feel like your knee will ‘give out’ on you.
The Muscles:
The knee joint is surrounded by A LOT of muscles, both above and below it.
Furthermore, almost every muscle from the ribcage to your toes can affect proper functioning of the knee.
Therefore, an in-depth look at muscles deserves it’s own blog post (maybe in the future!), and will not be covered here.
That being said, a lot of knee pain is caused by protective muscles surrounding the knee (usually the hamstrings and calves).
Calming these muscles down usually helps knee pain quite a bit.
A Word on Rehabilitation and Surgery
Most knee injuries do very well with proper physiotherapy and do not require surgery.
That being said, surgery is often done on people who have experienced a complete rupture of their ACL or PCL.
However, as newer research is conducted, more people might opt to forgo surgery and focus on proper rehabilitation, as return-to-sport rates have been found to be similar in operative and non-operative cases (1).
In either case, an individualized approach, and physiotherapy are very necessary. ACL and PCL injuries that are not complete ruptures are treated conservatively with physiotherapy.
Surgery is rare when only the MCL or LCL is injured. This is because they have good blood supply, and usually heal well without surgery.
Physiotherapy in Kitchener will be your best option.
Traumatic meniscal injuries that cause large tears and present with lots of pain/catching/locking sometimes lead to surgery if physiotherapy for 6-8 weeks was ineffective. Most meniscal injuries are managed well with proper physiotherapy, as large tears usually only happen with significant traumatic events (i.e. car accident, aggressive football tackles).
Conclusion
Hopefully by reading this post, the ‘simple’ knee joint has become much simpler.
If you have sustained a knee injury, or have knee pain, it’s highly possible that all of the above-mentioned structures are completely fine, as many other things (i.e. arthritis, knee-cap gliding issues, or muscular issues), can also cause pain. When you’re in pain, your best bet will be to get an individualized, thorough assessment by a trusted physiotherapist.
At Strive Physiotherapy and Performance, we are committed to providing an in-depth assessment to ensure we can work together to find the best plan of action for each individual client.
Call us at 519-895-2020, or use our online booking tool on www.strivept.ca to book an appointment with one of our knowledgeable physiotherapists, and they will be sure to help you understand your injury.
Take care,
Tyler Allen
Physiotherapist at Strive Physiotherapy & Performance